Zongwei Zhou
CrossPan: A Comprehensive Benchmark for Cross-Sequence Pancreas MRI Segmentation and Generalization
Apr 20, 2026Abstract:Automatic pancreas segmentation is fundamental to abdominal MRI analysis, yet deep learning models trained on one MRI sequence often fail catastrophically when applied to another-a challenge that has received little systematic investigation. We introduce CrossPan, a multi-institutional benchmark comprising 1,386 3D scans across three routinely acquired sequences (T1-weighted, T2-weighted, and Out-of-Phase) from eight centers. Our experiments reveal three key findings. First, cross-sequence domain shifts are far more severe than cross-center variability: models achieving Dice scores above 0.85 in-domain collapse to near-zero (<0.02) when transferred across sequences. Second, state-of-the-art domain generalization methods provide negligible benefit under these physics-driven contrast inversions, whereas foundation models like MedSAM2 maintain moderate zero-shot performance through contrast-invariant shape priors. Third, semi-supervised learning offers gains only under stable intensity distributions and becomes unstable on sequences with high intra-organ variability. These results establish cross-sequence generalization-not model architecture or center diversity-as the primary barrier to clinically deployable pancreas MRI segmentation. Dataset and code are available at https://crosspan.netlify.app/.
Distilling Photon-Counting CT into Routine Chest CT through Clinically Validated Degradation Modeling
Apr 08, 2026Abstract:Photon-counting CT (PCCT) provides superior image quality with higher spatial resolution and lower noise compared to conventional energy-integrating CT (EICT), but its limited clinical availability restricts large-scale research and clinical deployment. To bridge this gap, we propose SUMI, a simulated degradation-to-enhancement method that learns to reverse realistic acquisition artifacts in low-quality EICT by leveraging high-quality PCCT as reference. Our central insight is to explicitly model realistic acquisition degradations, transforming PCCT into clinically plausible lower-quality counterparts and learning to invert this process. The simulated degradations were validated for clinical realism by board-certified radiologists, enabling faithful supervision without requiring paired acquisitions at scale. As outcomes of this technical contribution, we: (1) train a latent diffusion model on 1,046 PCCTs, using an autoencoder first pre-trained on both these PCCTs and 405,379 EICTs from 145 hospitals to extract general CT latent features that we release for reuse in other generative medical imaging tasks; (2) construct a large-scale dataset of over 17,316 publicly available EICTs enhanced to PCCT-like quality, with radiologist-validated voxel-wise annotations of airway trees, arteries, veins, lungs, and lobes; and (3) demonstrate substantial improvements: across external data, SUMI outperforms state-of-the-art image translation methods by 15% in SSIM and 20% in PSNR, improves radiologist-rated clinical utility in reader studies, and enhances downstream top-ranking lesion detection performance, increasing sensitivity by up to 15% and F1 score by up to 10%. Our results suggest that emerging imaging advances can be systematically distilled into routine EICT using limited high-quality scans as reference.
Project Imaging-X: A Survey of 1000+ Open-Access Medical Imaging Datasets for Foundation Model Development
Mar 29, 2026Abstract:Foundation models have demonstrated remarkable success across diverse domains and tasks, primarily due to the thrive of large-scale, diverse, and high-quality datasets. However, in the field of medical imaging, the curation and assembling of such medical datasets are highly challenging due to the reliance on clinical expertise and strict ethical and privacy constraints, resulting in a scarcity of large-scale unified medical datasets and hindering the development of powerful medical foundation models. In this work, we present the largest survey to date of medical image datasets, covering over 1,000 open-access datasets with a systematic catalog of their modalities, tasks, anatomies, annotations, limitations, and potential for integration. Our analysis exposes a landscape that is modest in scale, fragmented across narrowly scoped tasks, and unevenly distributed across organs and modalities, which in turn limits the utility of existing medical image datasets for developing versatile and robust medical foundation models. To turn fragmentation into scale, we propose a metadata-driven fusion paradigm (MDFP) that integrates public datasets with shared modalities or tasks, thereby transforming multiple small data silos into larger, more coherent resources. Building on MDFP, we release an interactive discovery portal that enables end-to-end, automated medical image dataset integration, and compile all surveyed datasets into a unified, structured table that clearly summarizes their key characteristics and provides reference links, offering the community an accessible and comprehensive repository. By charting the current terrain and offering a principled path to dataset consolidation, our survey provides a practical roadmap for scaling medical imaging corpora, supporting faster data discovery, more principled dataset creation, and more capable medical foundation models.
Meissa: Multi-modal Medical Agentic Intelligence
Mar 09, 2026Abstract:Multi-modal large language models (MM-LLMs) have shown strong performance in medical image understanding and clinical reasoning. Recent medical agent systems extend them with tool use and multi-agent collaboration, enabling complex decision-making. However, these systems rely almost entirely on frontier models (e.g., GPT), whose API-based deployment incurs high cost, high latency, and privacy risks that conflict with on-premise clinical requirements. We present Meissa, a lightweight 4B-parameter medical MM-LLM that brings agentic capability offline. Instead of imitating static answers, Meissa learns both when to engage external interaction (strategy selection) and how to execute multi-step interaction (strategy execution) by distilling structured trajectories from frontier models. Specifically, we propose: (1) Unified trajectory modeling: trajectories (reasoning and action traces) are represented within a single state-action-observation formalism, allowing one model to generalize across heterogeneous medical environments. (2) Three-tier stratified supervision: the model's own errors trigger progressive escalation from direct reasoning to tool-augmented and multi-agent interaction, explicitly learning difficulty-aware strategy selection. (3) Prospective-retrospective supervision: pairing exploratory forward traces with hindsight-rationalized execution traces enables stable learning of effective interaction policies. Trained on 40K curated trajectories, Meissa matches or exceeds proprietary frontier agents in 10 of 16 evaluation settings across 13 medical benchmarks spanning radiology, pathology, and clinical reasoning. Using over 25x fewer parameters than typical frontier models like Gemini-3, Meissa operates fully offline with 22x lower end-to-end latency compared to API-based deployment. Data, models, and environments are released at https://github.com/Schuture/Meissa.
Early and Prediagnostic Detection of Pancreatic Cancer from Computed Tomography
Jan 29, 2026Abstract:Pancreatic ductal adenocarcinoma (PDAC), one of the deadliest solid malignancies, is often detected at a late and inoperable stage. Retrospective reviews of prediagnostic CT scans, when conducted by expert radiologists aware that the patient later developed PDAC, frequently reveal lesions that were previously overlooked. To help detecting these lesions earlier, we developed an automated system named ePAI (early Pancreatic cancer detection with Artificial Intelligence). It was trained on data from 1,598 patients from a single medical center. In the internal test involving 1,009 patients, ePAI achieved an area under the receiver operating characteristic curve (AUC) of 0.939-0.999, a sensitivity of 95.3%, and a specificity of 98.7% for detecting small PDAC less than 2 cm in diameter, precisely localizing PDAC as small as 2 mm. In an external test involving 7,158 patients across 6 centers, ePAI achieved an AUC of 0.918-0.945, a sensitivity of 91.5%, and a specificity of 88.0%, precisely localizing PDAC as small as 5 mm. Importantly, ePAI detected PDACs on prediagnostic CT scans obtained 3 to 36 months before clinical diagnosis that had originally been overlooked by radiologists. It successfully detected and localized PDACs in 75 of 159 patients, with a median lead time of 347 days before clinical diagnosis. Our multi-reader study showed that ePAI significantly outperformed 30 board-certified radiologists by 50.3% (P < 0.05) in sensitivity while maintaining a comparable specificity of 95.4% in detecting PDACs early and prediagnostic. These findings suggest its potential of ePAI as an assistive tool to improve early detection of pancreatic cancer.
Large-Scale Label Quality Assessment for Medical Segmentation via a Vision-Language Judge and Synthetic Data
Jan 20, 2026Abstract:Large-scale medical segmentation datasets often combine manual and pseudo-labels of uneven quality, which can compromise training and evaluation. Low-quality labels may hamper performance and make the model training less robust. To address this issue, we propose SegAE (Segmentation Assessment Engine), a lightweight vision-language model (VLM) that automatically predicts label quality across 142 anatomical structures. Trained on over four million image-label pairs with quality scores, SegAE achieves a high correlation coefficient of 0.902 with ground-truth Dice similarity and evaluates a 3D mask in 0.06s. SegAE shows several practical benefits: (I) Our analysis reveals widespread low-quality labeling across public datasets; (II) SegAE improves data efficiency and training performance in active and semi-supervised learning, reducing dataset annotation cost by one-third and quality-checking time by 70% per label. This tool provides a simple and effective solution for quality control in large-scale medical segmentation datasets. The dataset, model weights, and codes are released at https://github.com/Schuture/SegAE.
Auditing Significance, Metric Choice, and Demographic Fairness in Medical AI Challenges
Dec 22, 2025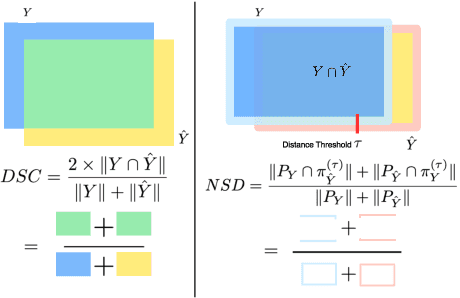
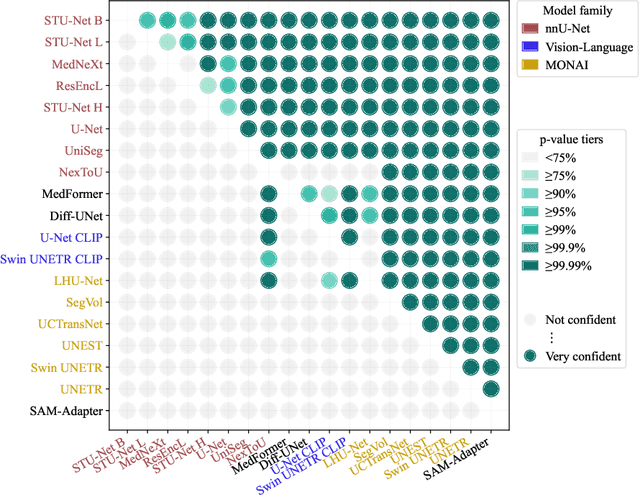
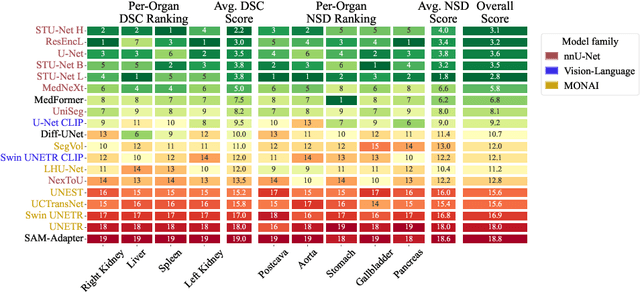
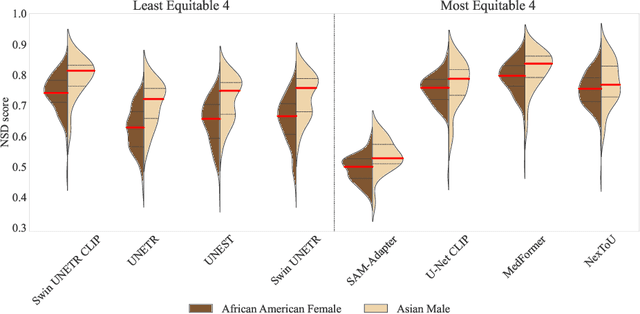
Abstract:Open challenges have become the de facto standard for comparative ranking of medical AI methods. Despite their importance, medical AI leaderboards exhibit three persistent limitations: (1) score gaps are rarely tested for statistical significance, so rank stability is unknown; (2) single averaged metrics are applied to every organ, hiding clinically important boundary errors; (3) performance across intersecting demographics is seldom reported, masking fairness and equity gaps. We introduce RankInsight, an open-source toolkit that seeks to address these limitations. RankInsight (1) computes pair-wise significance maps that show the nnU-Net family outperforms Vision-Language and MONAI submissions with high statistical certainty; (2) recomputes leaderboards with organ-appropriate metrics, reversing the order of the top four models when Dice is replaced by NSD for tubular structures; and (3) audits intersectional fairness, revealing that more than half of the MONAI-based entries have the largest gender-race discrepancy on our proprietary Johns Hopkins Hospital dataset. The RankInsight toolkit is publicly released and can be directly applied to past, ongoing, and future challenges. It enables organizers and participants to publish rankings that are statistically sound, clinically meaningful, and demographically fair.
See More, Change Less: Anatomy-Aware Diffusion for Contrast Enhancement
Dec 08, 2025Abstract:Image enhancement improves visual quality and helps reveal details that are hard to see in the original image. In medical imaging, it can support clinical decision-making, but current models often over-edit. This can distort organs, create false findings, and miss small tumors because these models do not understand anatomy or contrast dynamics. We propose SMILE, an anatomy-aware diffusion model that learns how organs are shaped and how they take up contrast. It enhances only clinically relevant regions while leaving all other areas unchanged. SMILE introduces three key ideas: (1) structure-aware supervision that follows true organ boundaries and contrast patterns; (2) registration-free learning that works directly with unaligned multi-phase CT scans; (3) unified inference that provides fast and consistent enhancement across all contrast phases. Across six external datasets, SMILE outperforms existing methods in image quality (14.2% higher SSIM, 20.6% higher PSNR, 50% better FID) and in clinical usefulness by producing anatomically accurate and diagnostically meaningful images. SMILE also improves cancer detection from non-contrast CT, raising the F1 score by up to 10 percent.
PanTS: The Pancreatic Tumor Segmentation Dataset
Jul 02, 2025Abstract:PanTS is a large-scale, multi-institutional dataset curated to advance research in pancreatic CT analysis. It contains 36,390 CT scans from 145 medical centers, with expert-validated, voxel-wise annotations of over 993,000 anatomical structures, covering pancreatic tumors, pancreas head, body, and tail, and 24 surrounding anatomical structures such as vascular/skeletal structures and abdominal/thoracic organs. Each scan includes metadata such as patient age, sex, diagnosis, contrast phase, in-plane spacing, slice thickness, etc. AI models trained on PanTS achieve significantly better performance in pancreatic tumor detection, localization, and segmentation compared to those trained on existing public datasets. Our analysis indicates that these gains are directly attributable to the 16x larger-scale tumor annotations and indirectly supported by the 24 additional surrounding anatomical structures. As the largest and most comprehensive resource of its kind, PanTS offers a new benchmark for developing and evaluating AI models in pancreatic CT analysis.
Are Vision Language Models Ready for Clinical Diagnosis? A 3D Medical Benchmark for Tumor-centric Visual Question Answering
May 25, 2025Abstract:Vision-Language Models (VLMs) have shown promise in various 2D visual tasks, yet their readiness for 3D clinical diagnosis remains unclear due to stringent demands for recognition precision, reasoning ability, and domain knowledge. To systematically evaluate these dimensions, we present DeepTumorVQA, a diagnostic visual question answering (VQA) benchmark targeting abdominal tumors in CT scans. It comprises 9,262 CT volumes (3.7M slices) from 17 public datasets, with 395K expert-level questions spanning four categories: Recognition, Measurement, Visual Reasoning, and Medical Reasoning. DeepTumorVQA introduces unique challenges, including small tumor detection and clinical reasoning across 3D anatomy. Benchmarking four advanced VLMs (RadFM, M3D, Merlin, CT-CHAT), we find current models perform adequately on measurement tasks but struggle with lesion recognition and reasoning, and are still not meeting clinical needs. Two key insights emerge: (1) large-scale multimodal pretraining plays a crucial role in DeepTumorVQA testing performance, making RadFM stand out among all VLMs. (2) Our dataset exposes critical differences in VLM components, where proper image preprocessing and design of vision modules significantly affect 3D perception. To facilitate medical multimodal research, we have released DeepTumorVQA as a rigorous benchmark: https://github.com/Schuture/DeepTumorVQA.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge