M. Jorge Cardoso
School of Biomedical Engineering and Imaging Science, King's College London, UK
Cortical Surface Diffusion Generative Models
Feb 07, 2024Abstract:Cortical surface analysis has gained increased prominence, given its potential implications for neurological and developmental disorders. Traditional vision diffusion models, while effective in generating natural images, present limitations in capturing intricate development patterns in neuroimaging due to limited datasets. This is particularly true for generating cortical surfaces where individual variability in cortical morphology is high, leading to an urgent need for better methods to model brain development and diverse variability inherent across different individuals. In this work, we proposed a novel diffusion model for the generation of cortical surface metrics, using modified surface vision transformers as the principal architecture. We validate our method in the developing Human Connectome Project (dHCP), the results suggest our model demonstrates superior performance in capturing the intricate details of evolving cortical surfaces. Furthermore, our model can generate high-quality realistic samples of cortical surfaces conditioned on postmenstrual age(PMA) at scan.
RAISE -- Radiology AI Safety, an End-to-end lifecycle approach
Nov 24, 2023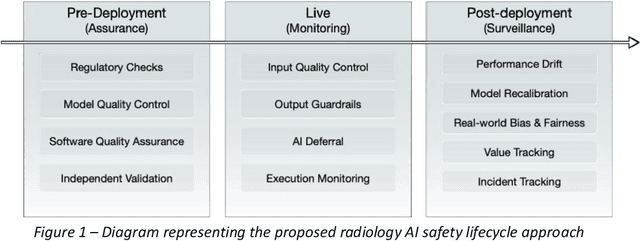
Abstract:The integration of AI into radiology introduces opportunities for improved clinical care provision and efficiency but it demands a meticulous approach to mitigate potential risks as with any other new technology. Beginning with rigorous pre-deployment evaluation and validation, the focus should be on ensuring models meet the highest standards of safety, effectiveness and efficacy for their intended applications. Input and output guardrails implemented during production usage act as an additional layer of protection, identifying and addressing individual failures as they occur. Continuous post-deployment monitoring allows for tracking population-level performance (data drift), fairness, and value delivery over time. Scheduling reviews of post-deployment model performance and educating radiologists about new algorithmic-driven findings is critical for AI to be effective in clinical practice. Recognizing that no single AI solution can provide absolute assurance even when limited to its intended use, the synergistic application of quality assurance at multiple levels - regulatory, clinical, technical, and ethical - is emphasized. Collaborative efforts between stakeholders spanning healthcare systems, industry, academia, and government are imperative to address the multifaceted challenges involved. Trust in AI is an earned privilege, contingent on a broad set of goals, among them transparently demonstrating that the AI adheres to the same rigorous safety, effectiveness and efficacy standards as other established medical technologies. By doing so, developers can instil confidence among providers and patients alike, enabling the responsible scaling of AI and the realization of its potential benefits. The roadmap presented herein aims to expedite the achievement of deployable, reliable, and safe AI in radiology.
A 3D generative model of pathological multi-modal MR images and segmentations
Nov 08, 2023Abstract:Generative modelling and synthetic data can be a surrogate for real medical imaging datasets, whose scarcity and difficulty to share can be a nuisance when delivering accurate deep learning models for healthcare applications. In recent years, there has been an increased interest in using these models for data augmentation and synthetic data sharing, using architectures such as generative adversarial networks (GANs) or diffusion models (DMs). Nonetheless, the application of synthetic data to tasks such as 3D magnetic resonance imaging (MRI) segmentation remains limited due to the lack of labels associated with the generated images. Moreover, many of the proposed generative MRI models lack the ability to generate arbitrary modalities due to the absence of explicit contrast conditioning. These limitations prevent the user from adjusting the contrast and content of the images and obtaining more generalisable data for training task-specific models. In this work, we propose brainSPADE3D, a 3D generative model for brain MRI and associated segmentations, where the user can condition on specific pathological phenotypes and contrasts. The proposed joint imaging-segmentation generative model is shown to generate high-fidelity synthetic images and associated segmentations, with the ability to combine pathologies. We demonstrate how the model can alleviate issues with segmentation model performance when unexpected pathologies are present in the data.
InverseSR: 3D Brain MRI Super-Resolution Using a Latent Diffusion Model
Aug 23, 2023



Abstract:High-resolution (HR) MRI scans obtained from research-grade medical centers provide precise information about imaged tissues. However, routine clinical MRI scans are typically in low-resolution (LR) and vary greatly in contrast and spatial resolution due to the adjustments of the scanning parameters to the local needs of the medical center. End-to-end deep learning methods for MRI super-resolution (SR) have been proposed, but they require re-training each time there is a shift in the input distribution. To address this issue, we propose a novel approach that leverages a state-of-the-art 3D brain generative model, the latent diffusion model (LDM) trained on UK BioBank, to increase the resolution of clinical MRI scans. The LDM acts as a generative prior, which has the ability to capture the prior distribution of 3D T1-weighted brain MRI. Based on the architecture of the brain LDM, we find that different methods are suitable for different settings of MRI SR, and thus propose two novel strategies: 1) for SR with more sparsity, we invert through both the decoder of the LDM and also through a deterministic Denoising Diffusion Implicit Models (DDIM), an approach we will call InverseSR(LDM); 2) for SR with less sparsity, we invert only through the LDM decoder, an approach we will call InverseSR(Decoder). These two approaches search different latent spaces in the LDM model to find the optimal latent code to map the given LR MRI into HR. The training process of the generative model is independent of the MRI under-sampling process, ensuring the generalization of our method to many MRI SR problems with different input measurements. We validate our method on over 100 brain T1w MRIs from the IXI dataset. Our method can demonstrate that powerful priors given by LDM can be used for MRI reconstruction.
Generative AI for Medical Imaging: extending the MONAI Framework
Jul 27, 2023Abstract:Recent advances in generative AI have brought incredible breakthroughs in several areas, including medical imaging. These generative models have tremendous potential not only to help safely share medical data via synthetic datasets but also to perform an array of diverse applications, such as anomaly detection, image-to-image translation, denoising, and MRI reconstruction. However, due to the complexity of these models, their implementation and reproducibility can be difficult. This complexity can hinder progress, act as a use barrier, and dissuade the comparison of new methods with existing works. In this study, we present MONAI Generative Models, a freely available open-source platform that allows researchers and developers to easily train, evaluate, and deploy generative models and related applications. Our platform reproduces state-of-art studies in a standardised way involving different architectures (such as diffusion models, autoregressive transformers, and GANs), and provides pre-trained models for the community. We have implemented these models in a generalisable fashion, illustrating that their results can be extended to 2D or 3D scenarios, including medical images with different modalities (like CT, MRI, and X-Ray data) and from different anatomical areas. Finally, we adopt a modular and extensible approach, ensuring long-term maintainability and the extension of current applications for future features.
Unsupervised 3D out-of-distribution detection with latent diffusion models
Jul 07, 2023


Abstract:Methods for out-of-distribution (OOD) detection that scale to 3D data are crucial components of any real-world clinical deep learning system. Classic denoising diffusion probabilistic models (DDPMs) have been recently proposed as a robust way to perform reconstruction-based OOD detection on 2D datasets, but do not trivially scale to 3D data. In this work, we propose to use Latent Diffusion Models (LDMs), which enable the scaling of DDPMs to high-resolution 3D medical data. We validate the proposed approach on near- and far-OOD datasets and compare it to a recently proposed, 3D-enabled approach using Latent Transformer Models (LTMs). Not only does the proposed LDM-based approach achieve statistically significant better performance, it also shows less sensitivity to the underlying latent representation, more favourable memory scaling, and produces better spatial anomaly maps. Code is available at https://github.com/marksgraham/ddpm-ood
DeepEdit: Deep Editable Learning for Interactive Segmentation of 3D Medical Images
May 18, 2023Abstract:Automatic segmentation of medical images is a key step for diagnostic and interventional tasks. However, achieving this requires large amounts of annotated volumes, which can be tedious and time-consuming task for expert annotators. In this paper, we introduce DeepEdit, a deep learning-based method for volumetric medical image annotation, that allows automatic and semi-automatic segmentation, and click-based refinement. DeepEdit combines the power of two methods: a non-interactive (i.e. automatic segmentation using nnU-Net, UNET or UNETR) and an interactive segmentation method (i.e. DeepGrow), into a single deep learning model. It allows easy integration of uncertainty-based ranking strategies (i.e. aleatoric and epistemic uncertainty computation) and active learning. We propose and implement a method for training DeepEdit by using standard training combined with user interaction simulation. Once trained, DeepEdit allows clinicians to quickly segment their datasets by using the algorithm in auto segmentation mode or by providing clicks via a user interface (i.e. 3D Slicer, OHIF). We show the value of DeepEdit through evaluation on the PROSTATEx dataset for prostate/prostatic lesions and the Multi-Atlas Labeling Beyond the Cranial Vault (BTCV) dataset for abdominal CT segmentation, using state-of-the-art network architectures as baseline for comparison. DeepEdit could reduce the time and effort annotating 3D medical images compared to DeepGrow alone. Source code is available at https://github.com/Project-MONAI/MONAILabel
Cross Attention Transformers for Multi-modal Unsupervised Whole-Body PET Anomaly Detection
Apr 14, 2023Abstract:Cancer is a highly heterogeneous condition that can occur almost anywhere in the human body. 18F-fluorodeoxyglucose is an imaging modality commonly used to detect cancer due to its high sensitivity and clear visualisation of the pattern of metabolic activity. Nonetheless, as cancer is highly heterogeneous, it is challenging to train general-purpose discriminative cancer detection models, with data availability and disease complexity often cited as a limiting factor. Unsupervised anomaly detection models have been suggested as a putative solution. These models learn a healthy representation of tissue and detect cancer by predicting deviations from the healthy norm, which requires models capable of accurately learning long-range interactions between organs and their imaging patterns with high levels of expressivity. Such characteristics are suitably satisfied by transformers, which have been shown to generate state-of-the-art results in unsupervised anomaly detection by training on normal data. This work expands upon such approaches by introducing multi-modal conditioning of the transformer via cross-attention i.e. supplying anatomical reference from paired CT. Using 294 whole-body PET/CT samples, we show that our anomaly detection method is robust and capable of achieving accurate cancer localization results even in cases where normal training data is unavailable. In addition, we show the efficacy of this approach on out-of-sample data showcasing the generalizability of this approach with limited training data. Lastly, we propose to combine model uncertainty with a new kernel density estimation approach, and show that it provides clinically and statistically significant improvements when compared to the classic residual-based anomaly maps. Overall, a superior performance is demonstrated against leading state-of-the-art alternatives, drawing attention to the potential of these approaches.
* Accepted for publication at the Journal of Machine Learning for Biomedical Imaging (MELBA) https://melba-journal.org/2023:006
Understanding metric-related pitfalls in image analysis validation
Feb 09, 2023Abstract:Validation metrics are key for the reliable tracking of scientific progress and for bridging the current chasm between artificial intelligence (AI) research and its translation into practice. However, increasing evidence shows that particularly in image analysis, metrics are often chosen inadequately in relation to the underlying research problem. This could be attributed to a lack of accessibility of metric-related knowledge: While taking into account the individual strengths, weaknesses, and limitations of validation metrics is a critical prerequisite to making educated choices, the relevant knowledge is currently scattered and poorly accessible to individual researchers. Based on a multi-stage Delphi process conducted by a multidisciplinary expert consortium as well as extensive community feedback, the present work provides the first reliable and comprehensive common point of access to information on pitfalls related to validation metrics in image analysis. Focusing on biomedical image analysis but with the potential of transfer to other fields, the addressed pitfalls generalize across application domains and are categorized according to a newly created, domain-agnostic taxonomy. To facilitate comprehension, illustrations and specific examples accompany each pitfall. As a structured body of information accessible to researchers of all levels of expertise, this work enhances global comprehension of a key topic in image analysis validation.
Current State of Community-Driven Radiological AI Deployment in Medical Imaging
Dec 29, 2022



Abstract:Artificial Intelligence (AI) has become commonplace to solve routine everyday tasks. Because of the exponential growth in medical imaging data volume and complexity, the workload on radiologists is steadily increasing. We project that the gap between the number of imaging exams and the number of expert radiologist readers required to cover this increase will continue to expand, consequently introducing a demand for AI-based tools that improve the efficiency with which radiologists can comfortably interpret these exams. AI has been shown to improve efficiency in medical-image generation, processing, and interpretation, and a variety of such AI models have been developed across research labs worldwide. However, very few of these, if any, find their way into routine clinical use, a discrepancy that reflects the divide between AI research and successful AI translation. To address the barrier to clinical deployment, we have formed MONAI Consortium, an open-source community which is building standards for AI deployment in healthcare institutions, and developing tools and infrastructure to facilitate their implementation. This report represents several years of weekly discussions and hands-on problem solving experience by groups of industry experts and clinicians in the MONAI Consortium. We identify barriers between AI-model development in research labs and subsequent clinical deployment and propose solutions. Our report provides guidance on processes which take an imaging AI model from development to clinical implementation in a healthcare institution. We discuss various AI integration points in a clinical Radiology workflow. We also present a taxonomy of Radiology AI use-cases. Through this report, we intend to educate the stakeholders in healthcare and AI (AI researchers, radiologists, imaging informaticists, and regulators) about cross-disciplinary challenges and possible solutions.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge