Tanzeem Choudhury
Ethical Fairness without Demographics in Human-Centered AI
Mar 17, 2026Abstract:Computational models are increasingly embedded in human-centered domains such as healthcare, education, workplace analytics, and digital well-being, where their predictions directly influence individual outcomes and collective welfare. In such contexts, achieving high accuracy alone is insufficient; models must also act ethically and equitably across diverse populations. However, fair AI approaches that rely on demographic attributes are impractical, as such information is often unavailable, privacy-sensitive, or restricted by regulatory frameworks. Moreover, conventional parity-based fairness approaches, while aiming for equity, can inadvertently violate core ethical principles by trading off subgroup performance or stability. To address this challenge, we present Flare (Fisher-guided LAtent-subgroup learning with do-no-harm REgularization), the first demographic-agnostic framework that aligns algorithmic fairness with ethical principles through the geometry of optimization. Flare leverages Fisher Information to regularize curvature, uncovering latent disparities in model behavior without access to demographic or sensitive attributes. By integrating representation, loss, and curvature signals, it identifies hidden performance strata and adaptively refines them through collaborative but do-no-harm optimization, enhancing each subgroup's performance while preserving global stability and ethical balance. We also introduce BHE (Beneficence-Harm Avoidance-Equity), a novel metric suite that operationalizes ethical fairness evaluation beyond statistical parity. Extensive evaluations across diverse physiological (EDA), behavioral (IHS), and clinical (OhioT1DM) datasets show that Flare consistently enhances ethical fairness compared to state-of-the-art baselines.
Exploring Personalized Health Support through Data-Driven, Theory-Guided LLMs: A Case Study in Sleep Health
Feb 19, 2025Abstract:Despite the prevalence of sleep-tracking devices, many individuals struggle to translate data into actionable improvements in sleep health. Current methods often provide data-driven suggestions but may not be feasible and adaptive to real-life constraints and individual contexts. We present HealthGuru, a novel large language model-powered chatbot to enhance sleep health through data-driven, theory-guided, and adaptive recommendations with conversational behavior change support. HealthGuru's multi-agent framework integrates wearable device data, contextual information, and a contextual multi-armed bandit model to suggest tailored sleep-enhancing activities. The system facilitates natural conversations while incorporating data-driven insights and theoretical behavior change techniques. Our eight-week in-the-wild deployment study with 16 participants compared HealthGuru to a baseline chatbot. Results show improved metrics like sleep duration and activity scores, higher quality responses, and increased user motivation for behavior change with HealthGuru. We also identify challenges and design considerations for personalization and user engagement in health chatbots.
Patient-independent Schizophrenia Relapse Prediction Using Mobile Sensor based Daily Behavioral Rhythm Changes
Jun 25, 2021
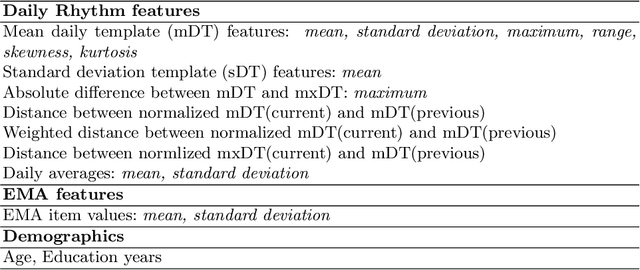

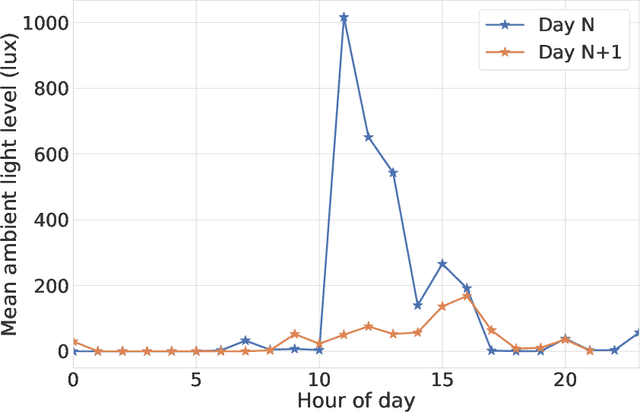
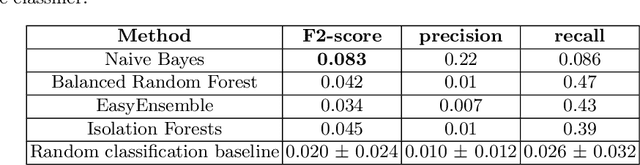
Abstract:A schizophrenia relapse has severe consequences for a patient's health, work, and sometimes even life safety. If an oncoming relapse can be predicted on time, for example by detecting early behavioral changes in patients, then interventions could be provided to prevent the relapse. In this work, we investigated a machine learning based schizophrenia relapse prediction model using mobile sensing data to characterize behavioral features. A patient-independent model providing sequential predictions, closely representing the clinical deployment scenario for relapse prediction, was evaluated. The model uses the mobile sensing data from the recent four weeks to predict an oncoming relapse in the next week. We used the behavioral rhythm features extracted from daily templates of mobile sensing data, self-reported symptoms collected via EMA (Ecological Momentary Assessment), and demographics to compare different classifiers for the relapse prediction. Naive Bayes based model gave the best results with an F2 score of 0.083 when evaluated in a dataset consisting of 63 schizophrenia patients, each monitored for up to a year. The obtained F2 score, though low, is better than the baseline performance of random classification (F2 score of 0.02 $\pm$ 0.024). Thus, mobile sensing has predictive value for detecting an oncoming relapse and needs further investigation to improve the current performance. Towards that end, further feature engineering and model personalization based on the behavioral idiosyncrasies of a patient could be helpful.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge