Maxence Wynen
Towards Brain MRI Foundation Models for the Clinic: Findings from the FOMO25 Challenge
Apr 13, 2026Abstract:Clinical deployment of automated brain MRI analysis faces a fundamental challenge: clinical data is heterogeneous and noisy, and high-quality labels are prohibitively costly to obtain. Self-supervised learning (SSL) can address this by leveraging the vast amounts of unlabeled data produced in clinical workflows to train robust \textit{foundation models} that adapt out-of-domain with minimal supervision. However, the development of foundation models for brain MRI has been limited by small pretraining datasets and in-domain benchmarking focused on high-quality, research-grade data. To address this gap, we organized the FOMO25 challenge as a satellite event at MICCAI 2025. FOMO25 provided participants with a large pretraining dataset, FOMO60K, and evaluated models on data sourced directly from clinical workflows in few-shot and out-of-domain settings. Tasks covered infarct classification, meningioma segmentation, and brain age regression, and considered both models trained on FOMO60K (method track) and any data (open track). Nineteen foundation models from sixteen teams were evaluated using a standardized containerized pipeline. Results show that (a) self-supervised pretraining improves generalization on clinical data under domain shift, with the strongest models trained \textit{out-of-domain} surpassing supervised baselines trained \textit{in-domain}. (b) No single pretraining objective benefits all tasks: MAE favors segmentation, hybrid reconstruction-contrastive objectives favor classification, and (c) strong performance was achieved by small pretrained models, and improvements from scaling model size and training duration did not yield reliable benefits.
From 100,000+ images to winning the first brain MRI foundation model challenges: Sharing lessons and models
Jan 19, 2026Abstract:Developing Foundation Models for medical image analysis is essential to overcome the unique challenges of radiological tasks. The first challenges of this kind for 3D brain MRI, SSL3D and FOMO25, were held at MICCAI 2025. Our solution ranked first in tracks of both contests. It relies on a U-Net CNN architecture combined with strategies leveraging anatomical priors and neuroimaging domain knowledge. Notably, our models trained 1-2 orders of magnitude faster and were 10 times smaller than competing transformer-based approaches. Models are available here: https://github.com/jbanusco/BrainFM4Challenges.
ConfLUNet: Multiple sclerosis lesion instance segmentation in presence of confluent lesions
May 28, 2025Abstract:Accurate lesion-level segmentation on MRI is critical for multiple sclerosis (MS) diagnosis, prognosis, and disease monitoring. However, current evaluation practices largely rely on semantic segmentation post-processed with connected components (CC), which cannot separate confluent lesions (aggregates of confluent lesion units, CLUs) due to reliance on spatial connectivity. To address this misalignment with clinical needs, we introduce formal definitions of CLUs and associated CLU-aware detection metrics, and include them in an exhaustive instance segmentation evaluation framework. Within this framework, we systematically evaluate CC and post-processing-based Automated Confluent Splitting (ACLS), the only existing methods for lesion instance segmentation in MS. Our analysis reveals that CC consistently underestimates CLU counts, while ACLS tends to oversplit lesions, leading to overestimated lesion counts and reduced precision. To overcome these limitations, we propose ConfLUNet, the first end-to-end instance segmentation framework for MS lesions. ConfLUNet jointly optimizes lesion detection and delineation from a single FLAIR image. Trained on 50 patients, ConfLUNet significantly outperforms CC and ACLS on the held-out test set (n=13) in instance segmentation (Panoptic Quality: 42.0% vs. 37.5%/36.8%; p = 0.017/0.005) and lesion detection (F1: 67.3% vs. 61.6%/59.9%; p = 0.028/0.013). For CLU detection, ConfLUNet achieves the highest F1[CLU] (81.5%), improving recall over CC (+12.5%, p = 0.015) and precision over ACLS (+31.2%, p = 0.003). By combining rigorous definitions, new CLU-aware metrics, a reproducible evaluation framework, and the first dedicated end-to-end model, this work lays the foundation for lesion instance segmentation in MS.
Cortical lesions, central vein sign, and paramagnetic rim lesions in multiple sclerosis: emerging machine learning techniques and future avenues
Jan 19, 2022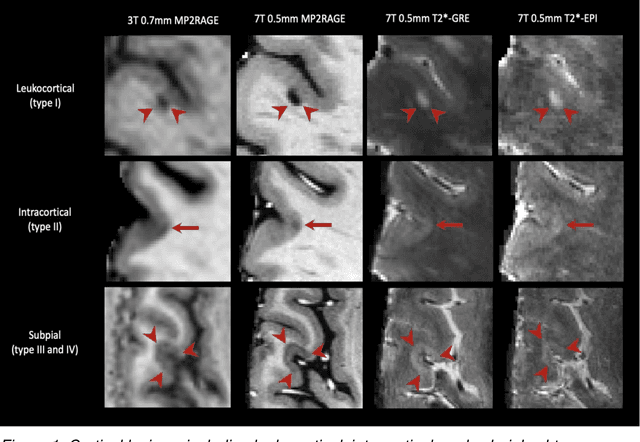
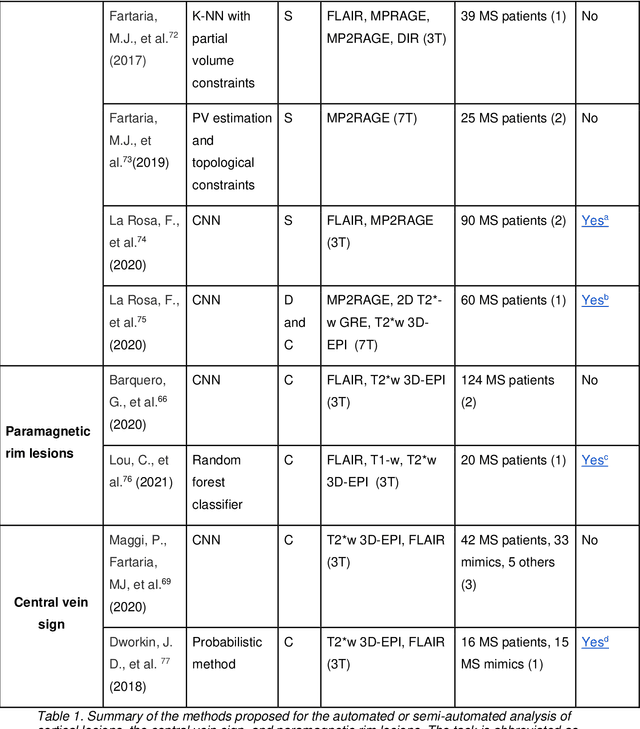
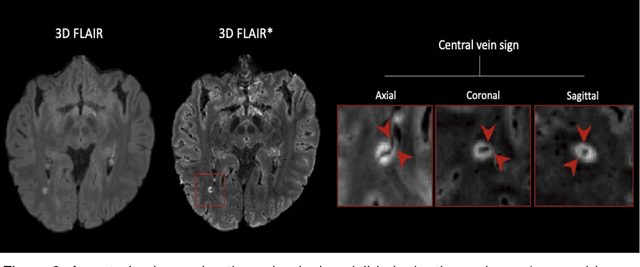
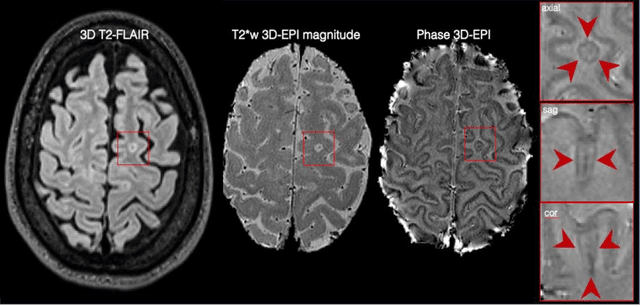
Abstract:The current multiple sclerosis (MS) diagnostic criteria lack specificity, and this may lead to misdiagnosis, which remains an issue in present-day clinical practice. In addition, conventional biomarkers only moderately correlate with MS disease progression. Recently, advanced MS lesional imaging biomarkers such as cortical lesions (CL), the central vein sign (CVS), and paramagnetic rim lesions (PRL), visible in specialized magnetic resonance imaging (MRI) sequences, have shown higher specificity in differential diagnosis. Moreover, studies have shown that CL and PRL are potential prognostic biomarkers, the former correlating with cognitive impairments and the latter with early disability progression. As machine learning-based methods have achieved extraordinary performance in the assessment of conventional imaging biomarkers, such as white matter lesion segmentation, several automated or semi-automated methods have been proposed for CL, CVS, and PRL as well. In the present review, we first introduce these advanced MS imaging biomarkers and their imaging methods. Subsequently, we describe the corresponding machine learning-based methods that were used to tackle these clinical questions, putting them into context with respect to the challenges they are still facing, including non-standardized MRI protocols, limited datasets, and moderate inter-rater variability. We conclude by presenting the current limitations that prevent their broader deployment and suggesting future research directions.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge