Daphna Raz
Ankle Exoskeletons May Hinder Standing Balance in Simple Models of Older and Younger Adults
Aug 14, 2024



Abstract:Humans rely on ankle torque to maintain standing balance, particularly in the presence of small to moderate perturbations. Reductions in maximum torque (MT) production and maximum rate of torque development (MRTD) occur at the ankle with age, diminishing stability. Ankle exoskeletons are powered orthotic devices that may assist older adults by compensating for reduced muscle force and power production capabilities. They may also be able to assist with ankle strategies used for balance. However, no studies have investigated the effect of such devices on balance in older adults. Here, we model the effect ankle exoskeletons have on stability in physics-based models of healthy young and old adults, focusing on the mitigation of age-related deficits such as reduced MT and MRTD. We show that an ankle exoskeleton moderately reduces feasible stability boundaries in users who have full ankle strength. For individuals with age-related deficits, there is a trade-off. While exoskeletons augment stability in low velocity conditions, they reduce stability in some high velocity conditions. Our results suggest that well-established control strategies must still be experimentally validated in older adults.
Reachable Sets for Safe, Real-Time Manipulator Trajectory Design
Feb 05, 2020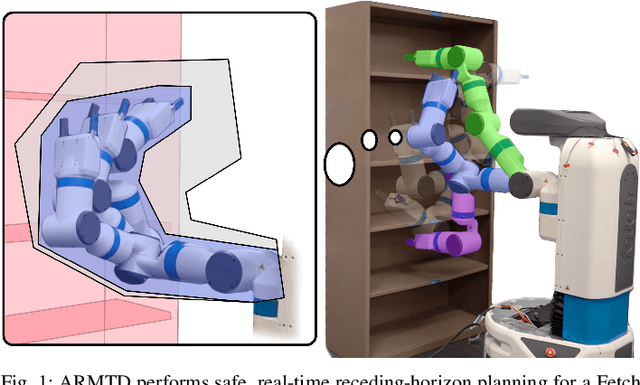
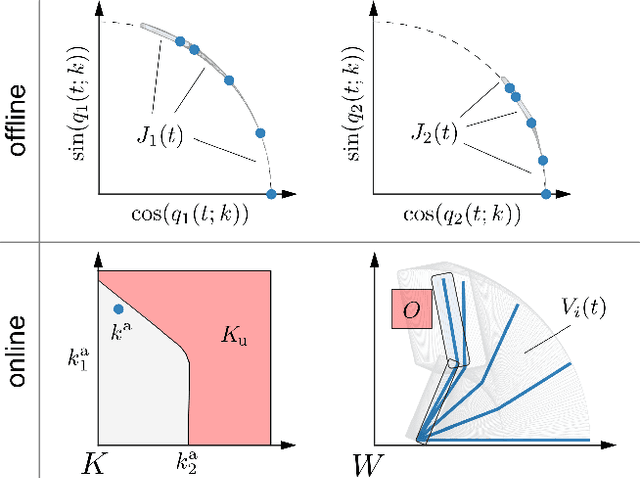
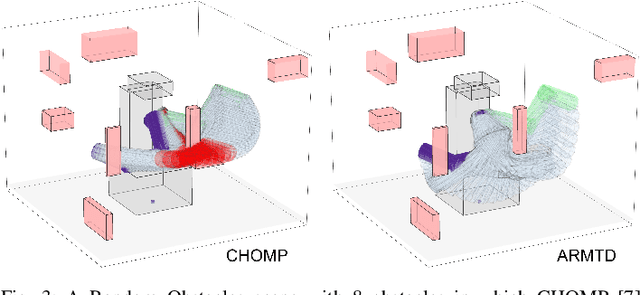
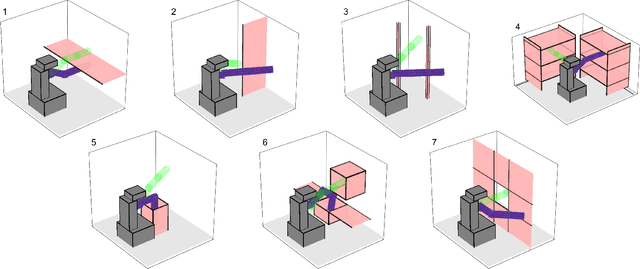
Abstract:For robotic arms to operate in arbitrary environments, especially near people, it is critical to certify the safety of their motion planning algorithms. However, there is often a trade-off between safety and real-time performance; one can either carefully design safe plans, or rapidly generate potentially-unsafe plans. This work presents a receding-horizon, real-time trajectory planner with safety guarantees, called ARMTD (Autonomous Reachability-based Manipulator Trajectory Design). The method first computes (offline) a reachable set of parameterized trajectories for each joint of an arm. Each trajectory includes a fail-safe maneuver (braking to a stop). At runtime, in each receding-horizon planning iteration, ARMTD constructs a reachable set of the entire arm in workspace and intersects it with obstacles to generate sub-differentiable and provably-conservative collision-avoidance constraints on the trajectory parameters. ARMTD then performs trajectory optimization for an arbitrary cost function on the parameters, subject to these constraints. On a 6 degree-of-freedom arm, ARMTD outperforms CHOMP in simulation and completes a variety of real-time planning tasks on hardware, all without collisions.
Automated Camera-Based Estimation of Rehabilitation Criteria Following ACL Reconstruction
Oct 25, 2018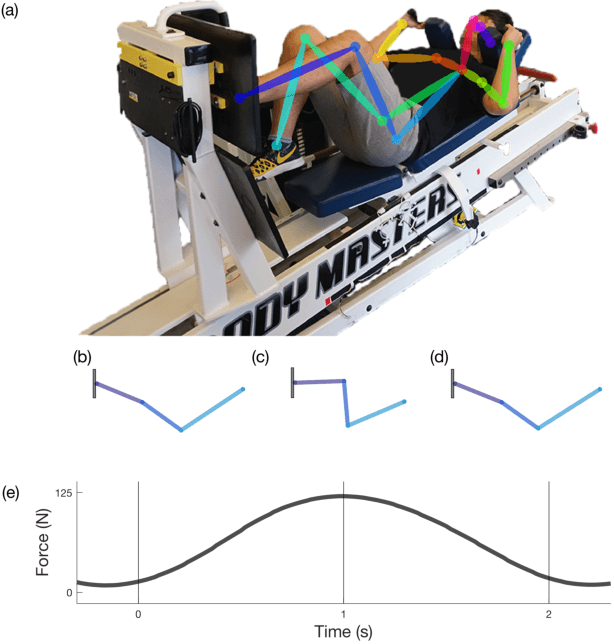
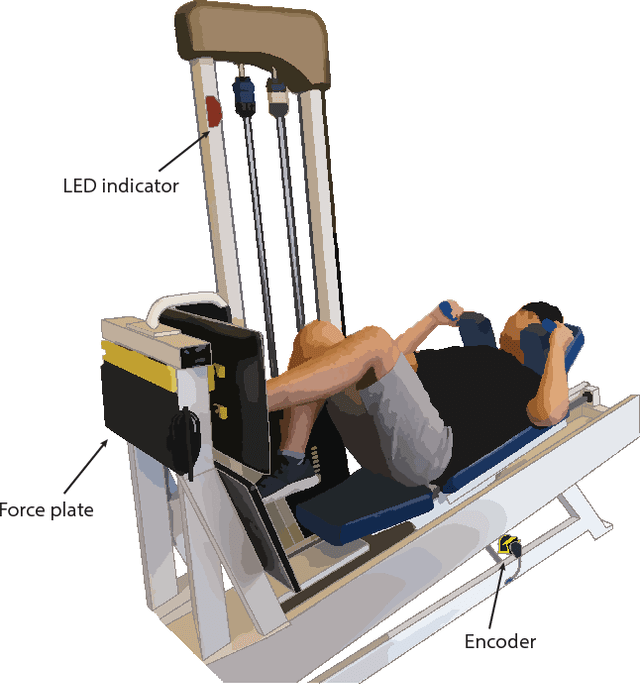
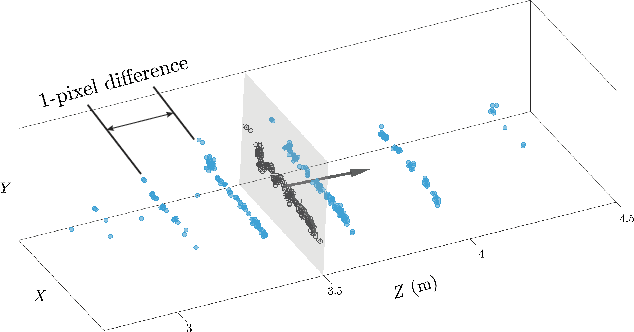
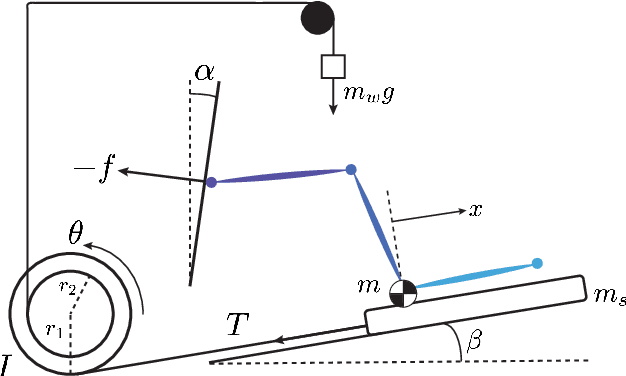
Abstract:Anterior cruciate ligament (ACL) reconstruction necessitates months of rehabilitation, during which a clinician evaluates whether a patient is ready to return to sports or occupation. Due to their time- and cost-intensive nature, these screenings to assess progress are unavailable to many. This paper introduces an automated, markerless, camera-based method for estimating rehabilitation criteria following ACL reconstruction. To evaluate the performance of this novel technique, data were collected weekly from 12 subjects as they used a leg press over the course of a 12-week rehabilitation period. The proposed camera-based method for estimating displacement and force was compared to encoder and force plate measurements. The leg press displacement and force values were estimated with 89.7% and 85.3% accuracy, respectively. These values were then used to calculate lower-limb symmetry and to track patient progress over time.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge