Joan C. Vilanova
The MAMA-MIA Challenge: Advancing Generalizability and Fairness in Breast MRI Tumor Segmentation and Treatment Response Prediction
Mar 01, 2026Abstract:Breast cancer is the most frequently diagnosed malignancy among women worldwide and a leading cause of cancer-related mortality. Dynamic contrast-enhanced magnetic resonance imaging plays a central role in tumor characterization and treatment monitoring, particularly in patients receiving neoadjuvant chemotherapy. However, existing artificial intelligence models for breast magnetic resonance imaging are often developed using single-center data and evaluated using aggregate performance metrics, limiting their generalizability and obscuring potential performance disparities across demographic subgroups. The MAMA-MIA Challenge was designed to address these limitations by introducing a large-scale benchmark that jointly evaluates primary tumor segmentation and prediction of pathologic complete response using pre-treatment magnetic resonance imaging only. The training cohort comprised 1,506 patients from multiple institutions in the United States, while evaluation was conducted on an external test set of 574 patients from three independent European centers to assess cross-continental and cross-institutional generalization. A unified scoring framework combined predictive performance with subgroup consistency across age, menopausal status, and breast density. Twenty-six international teams participated in the final evaluation phase. Results demonstrate substantial performance variability under external testing and reveal trade-offs between overall accuracy and subgroup fairness. The challenge provides standardized datasets, evaluation protocols, and public resources to promote the development of robust and equitable artificial intelligence systems for breast cancer imaging.
One-shot domain adaptation in multiple sclerosis lesion segmentation using convolutional neural networks
May 31, 2018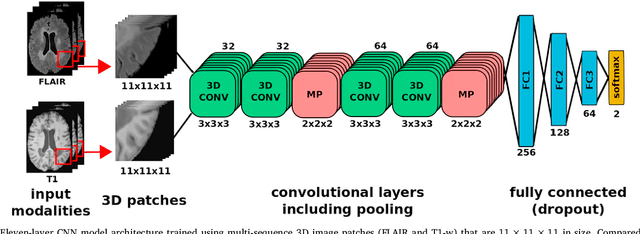
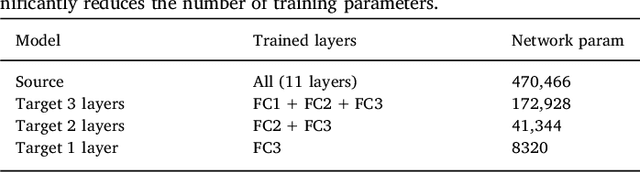

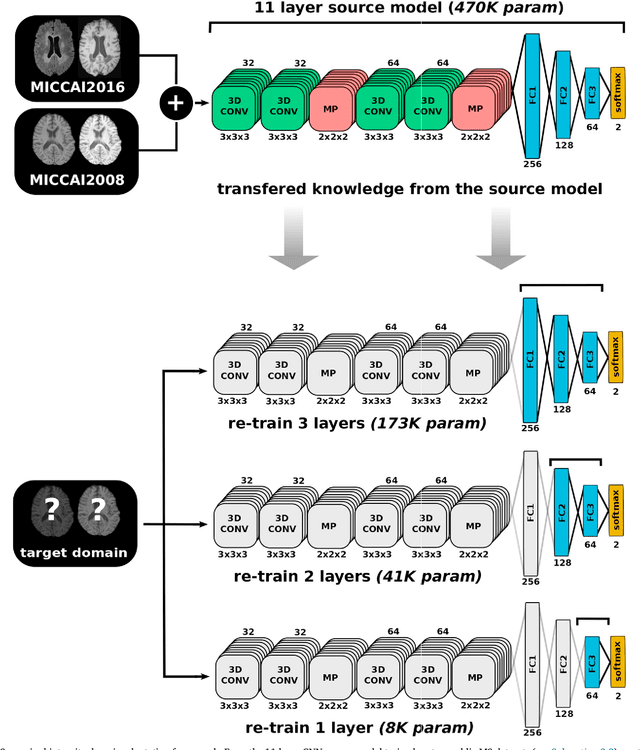
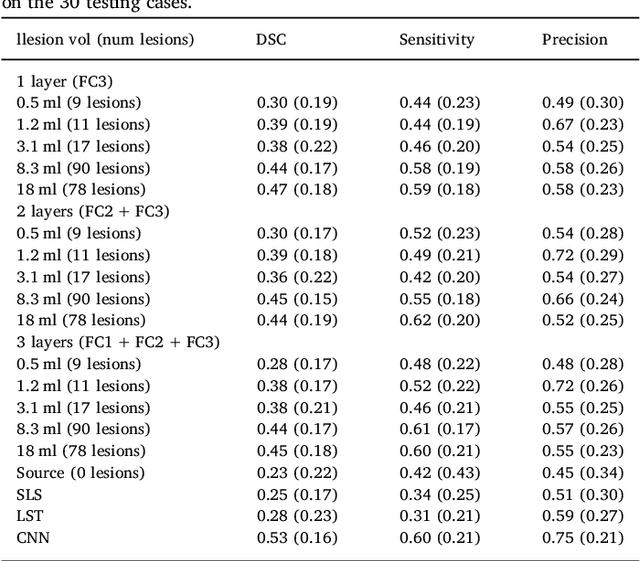
Abstract:In recent years, several convolutional neural network (CNN) methods have been proposed for the automated white matter lesion segmentation of multiple sclerosis (MS) patient images, due to their superior performance compared with those of other state-of-the-art methods. However, the accuracies of CNN methods tend to decrease significantly when evaluated on different image domains compared with those used for training, which demonstrates the lack of adaptability of CNNs to unseen imaging data. In this study, we analyzed the effect of intensity domain adaptation on our recently proposed CNN-based MS lesion segmentation method. Given a source model trained on two public MS datasets, we investigated the transferability of the CNN model when applied to other MRI scanners and protocols, evaluating the minimum number of annotated images needed from the new domain and the minimum number of layers needed to re-train to obtain comparable accuracy. Our analysis comprised MS patient data from both a clinical center and the public ISBI2015 challenge database, which permitted us to compare the domain adaptation capability of our model to that of other state-of-the-art methods. For the ISBI2015 challenge, our one-shot domain adaptation model trained using only a single image showed a performance similar to that of other CNN methods that were fully trained using the entire available training set, yielding a comparable human expert rater performance. We believe that our experiments will encourage the MS community to incorporate its use in different clinical settings with reduced amounts of annotated data. This approach could be meaningful not only in terms of the accuracy in delineating MS lesions but also in the related reductions in time and economic costs derived from manual lesion labeling.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge