Atle Bjørnerud
Examining Deployment and Refinement of the VIOLA-AI Intracranial Hemorrhage Model Using an Interactive NeoMedSys Platform
May 14, 2025Abstract:Background: There are many challenges and opportunities in the clinical deployment of AI tools in radiology. The current study describes a radiology software platform called NeoMedSys that can enable efficient deployment and refinements of AI models. We evaluated the feasibility and effectiveness of running NeoMedSys for three months in real-world clinical settings and focused on improvement performance of an in-house developed AI model (VIOLA-AI) designed for intracranial hemorrhage (ICH) detection. Methods: NeoMedSys integrates tools for deploying, testing, and optimizing AI models with a web-based medical image viewer, annotation system, and hospital-wide radiology information systems. A pragmatic investigation was deployed using clinical cases of patients presenting to the largest Emergency Department in Norway (site-1) with suspected traumatic brain injury (TBI) or patients with suspected stroke (site-2). We assessed ICH classification performance as VIOLA-AI encountered new data and underwent pre-planned model retraining. Performance metrics included sensitivity, specificity, accuracy, and the area under the receiver operating characteristic curve (AUC). Results: NeoMedSys facilitated iterative improvements in the AI model, significantly enhancing its diagnostic accuracy. Automated bleed detection and segmentation were reviewed in near real-time to facilitate re-training VIOLA-AI. The iterative refinement process yielded a marked improvement in classification sensitivity, rising to 90.3% (from 79.2%), and specificity that reached 89.3% (from 80.7%). The bleed detection ROC analysis for the entire sample demonstrated a high area-under-the-curve (AUC) of 0.949 (from 0.873). Model refinement stages were associated with notable gains, highlighting the value of real-time radiologist feedback.
MUSTER: Longitudinal Deformable Registration by Composition of Consecutive Deformations
Dec 19, 2024



Abstract:Longitudinal imaging allows for the study of structural changes over time. One approach to detecting such changes is by non-linear image registration. This study introduces Multi-Session Temporal Registration (MUSTER), a novel method that facilitates longitudinal analysis of changes in extended series of medical images. MUSTER improves upon conventional pairwise registration by incorporating more than two imaging sessions to recover longitudinal deformations. Longitudinal analysis at a voxel-level is challenging due to effects of a changing image contrast as well as instrumental and environmental sources of bias between sessions. We show that local normalized cross-correlation as an image similarity metric leads to biased results and propose a robust alternative. We test the performance of MUSTER on a synthetic multi-site, multi-session neuroimaging dataset and show that, in various scenarios, using MUSTER significantly enhances the estimated deformations relative to pairwise registration. Additionally, we apply MUSTER on a sample of older adults from the Alzheimer's Disease Neuroimaging Initiative (ADNI) study. The results show that MUSTER can effectively identify patterns of neuro-degeneration from T1-weighted images and that these changes correlate with changes in cognition, matching the performance of state of the art segmentation methods. By leveraging GPU acceleration, MUSTER efficiently handles large datasets, making it feasible also in situations with limited computational resources.
Deep Learning-based Intraoperative MRI Reconstruction
Jan 23, 2024Abstract:Purpose: To evaluate the quality of deep learning reconstruction for prospectively accelerated intraoperative magnetic resonance imaging (iMRI) during resective brain tumor surgery. Materials and Methods: Accelerated iMRI was performed during brain surgery using dual surface coils positioned around the area of resection. A deep learning (DL) model was trained on the fastMRI neuro dataset to mimic the data from the iMRI protocol. Evaluation was performed on imaging material from 40 patients imaged between 01.11.2021 - 01.06.2023 that underwent iMRI during tumor resection surgery. A comparative analysis was conducted between the conventional compressed sense (CS) method and the trained DL reconstruction method. Blinded evaluation of multiple image quality metrics was performed by two working neuro-radiologists and a working neurosurgeon on a 1 to 5 Likert scale (1=non diagnostic, 2=poor, 3=acceptable, 4=good, 5=excellent), and the favored reconstruction variant. Results: The DL reconstruction was strongly favored or favored over the CS reconstruction for 33/40, 39/40, and 8/40 of cases for reader 1, 2, and 3, respectively. Two of three readers consistently assigned higher ratings for the DL reconstructions, and the DL reconstructions had a higher score than their respective CS counterparts for 72%, 72%, and 14% of the cases for reader 1, 2, and 3, respectively. Still, the DL reconstructions exhibited shortcomings such as a striping artifact and reduced signal. Conclusion: DL shows promise to allow for high-quality reconstructions of intraoperative MRI with equal to or improved perceived spatial resolution, signal-to-noise ratio, diagnostic confidence, diagnostic conspicuity, and spatial resolution compared to compressed sense.
Treatment-aware Diffusion Probabilistic Model for Longitudinal MRI Generation and Diffuse Glioma Growth Prediction
Sep 14, 2023



Abstract:Diffuse gliomas are malignant brain tumors that grow widespread through the brain. The complex interactions between neoplastic cells and normal tissue, as well as the treatment-induced changes often encountered, make glioma tumor growth modeling challenging. In this paper, we present a novel end-to-end network capable of generating future tumor masks and realistic MRIs of how the tumor will look at any future time points for different treatment plans. Our approach is based on cutting-edge diffusion probabilistic models and deep-segmentation neural networks. We included sequential multi-parametric magnetic resonance images (MRI) and treatment information as conditioning inputs to guide the generative diffusion process. This allows for tumor growth estimates at any given time point. We trained the model using real-world postoperative longitudinal MRI data with glioma tumor growth trajectories represented as tumor segmentation maps over time. The model has demonstrated promising performance across a range of tasks, including the generation of high-quality synthetic MRIs with tumor masks, time-series tumor segmentations, and uncertainty estimates. Combined with the treatment-aware generated MRIs, the tumor growth predictions with uncertainty estimates can provide useful information for clinical decision-making.
Voxels Intersecting along Orthogonal Levels Attention U-Net (viola-Unet) to Segment Intracerebral Haemorrhage Using Computed Tomography Head Scans
Aug 12, 2022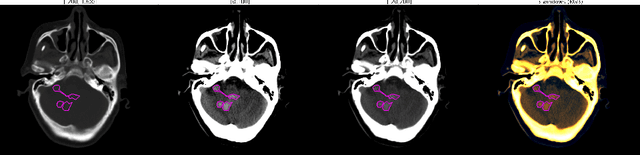
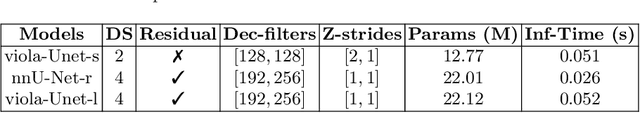
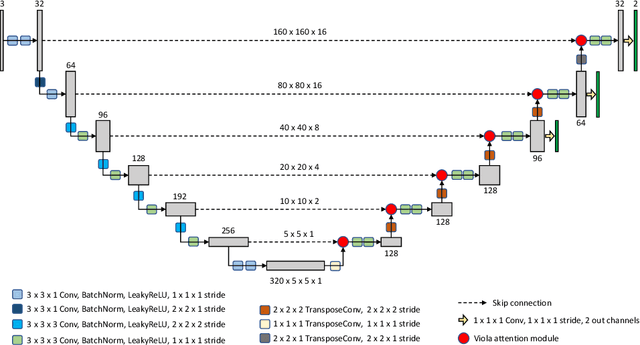
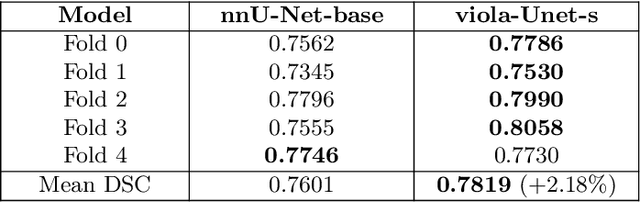
Abstract:We implemented two distinct 3-dimensional deep learning neural networks and evaluate their ability to segment intracranial hemorrhage (ICH) seen on non-contrast computed tomography (CT). One model, referred to as "Voxels-Intersecting along Orthogonal Levels of Attention U-Net" (viola-Unet), has architecture elements that are amenable to the INSTANCE 2022 Data Challenge. A second comparison model was derived from the no-new U-Net (nnU-Net). Input images and ground truth segmentation maps were used to train the two networks separately in supervised manner; validation data were subsequently used for semi-supervised training. Model predictions were compared during 5-fold cross validation. The viola-Unet outperformed the comparison network on two out of four performance metrics (i.e., NSD and RVD). An ensemble model that combined viola-Unet and nnU-Net networks had the highest performance for DSC and HD. We demonstrate there were ICH segmentation performance benefits associated with a 3D U-Net efficiently incorporates spatially orthogonal features during the decoding branch of the U-Net. The code base, pretrained weights, and docker image of the viola-Unet AI tool will be publicly available at https://github.com/samleoqh/Viola-Unet .
A Densely Interconnected Network for Deep Learning Accelerated MRI
Jul 05, 2022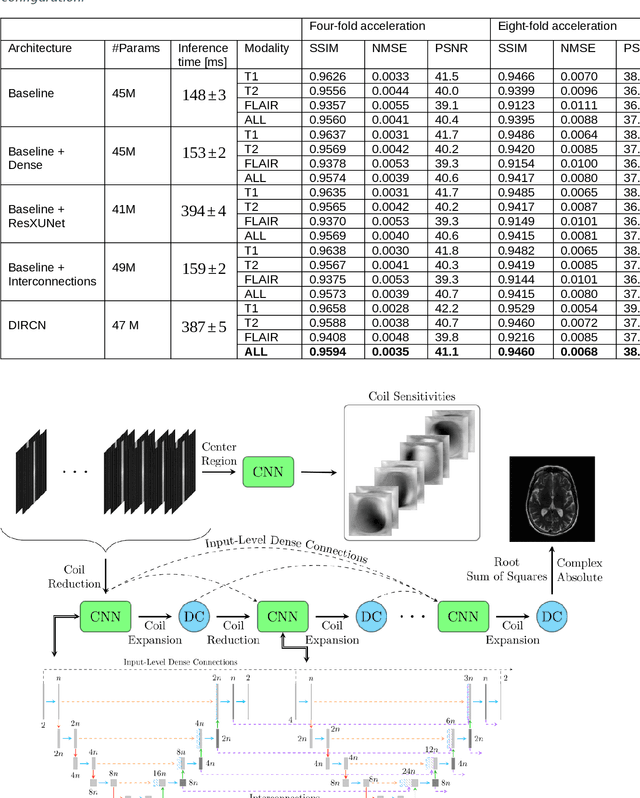
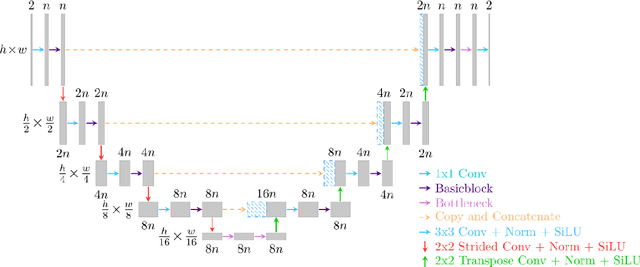
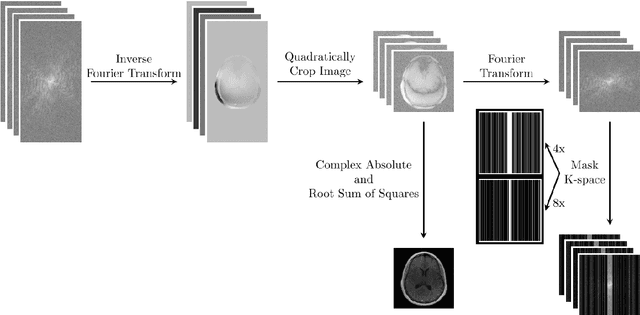
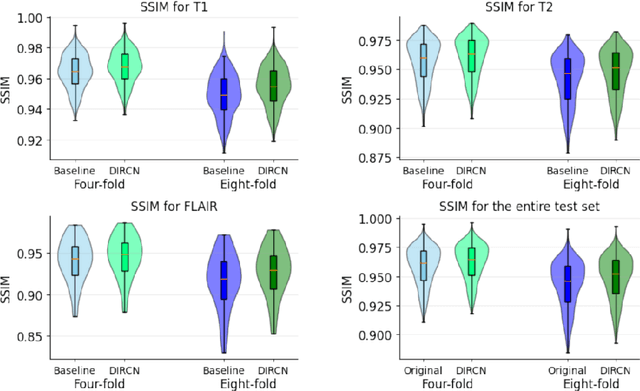
Abstract:Objective: To improve accelerated MRI reconstruction through a densely connected cascading deep learning reconstruction framework. Materials and Methods: A cascading deep learning reconstruction framework (baseline model) was modified by applying three architectural modifications: Input-level dense connections between cascade inputs and outputs, an improved deep learning sub-network, and long-range skip-connections between subsequent deep learning networks. An ablation study was performed, where five model configurations were trained on the NYU fastMRI neuro dataset with an end-to-end scheme conjunct on four- and eight-fold acceleration. The trained models were evaluated by comparing their respective structural similarity index measure (SSIM), normalized mean square error (NMSE) and peak signal to noise ratio (PSNR). Results: The proposed densely interconnected residual cascading network (DIRCN), utilizing all three suggested modifications, achieved a SSIM improvement of 8% and 11% for four- and eight-fold acceleration, respectively. For eight-fold acceleration, the model achieved a 23% decrease in the NMSE when compared to the baseline model. In an ablation study, the individual architectural modifications all contributed to this improvement, by reducing the SSIM and NMSE with approximately 3% and 5% for four-fold acceleration, respectively. Conclusion: The proposed architectural modifications allow for simple adjustments on an already existing cascading framework to further improve the resulting reconstructions.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge