William Le
AMO-ENE: Attention-based Multi-Omics Fusion Model for Outcome Prediction in Extra Nodal Extension and HPV-associated Oropharyngeal Cancer
Apr 10, 2026Abstract:Extranodal extension (ENE) is an emerging prognostic factor in human papillomavirus (HPV)-associated oropharyngeal cancer (OPC), although it is currently omitted as a clinical staging criteria. Recent works have advocated for the inclusion of iENE as a prognostic marker in HPV-positive OPC staging. However, several practical limitations continue to hinder its clinical integration, including inconsistencies in segmentation, low contrast in the periphery of metastatic lymph nodes on CT imaging, and laborious manual annotations. To address these limitations, we propose a fully automated end-to-end pipeline that uses computed tomography (CT) images with clinical data to assess the status of nodal ENE and predict treatment outcomes. Our approach includes a hierarchical 3D semi-supervised segmentation model designed to detect and delineate relevant iENE from radiotherapy planning CT scans. From these segmentations, a set of radiomics and deep features are extracted to train an imaging-detected ENE grading classifier. The predicted ENE status is then evaluated for its prognostic value and compared with existing staging criteria. Furthermore, we integrate these nodal features with primary tumor characteristics in a multimodal, attention-based outcome prediction model, providing a dynamic framework for outcome prediction. Our method is validated in an internal cohort of 397 HPV-positive OPC patients treated with radiation therapy or chemoradiotherapy between 2009 and 2020. For outcome prediction at the 2-year mark, our pipeline surpassed baseline models with 88.2% (4.8) in AUC for metastatic recurrence, 79.2% (7.4) for overall survival, and 78.1% (8.6) for disease-free survival. We also obtain a concordance index of 83.3% (6.5) for metastatic recurrence, 71.3% (8.9) for overall survival, and 70.0% (8.1) for disease-free survival, making it feasible for clinical decision making.
A Normalized Fully Convolutional Approach to Head and Neck Cancer Outcome Prediction
May 29, 2020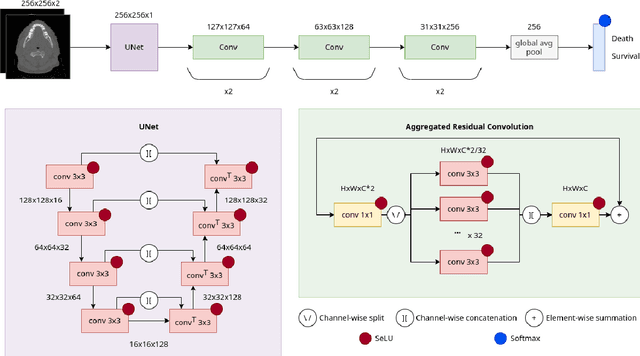

Abstract:In medical imaging, radiological scans of different modalities serve to enhance different sets of features for clinical diagnosis and treatment planning. This variety enriches the source information that could be used for outcome prediction. Deep learning methods are particularly well-suited for feature extraction from high-dimensional inputs such as images. In this work, we apply a CNN classification network augmented with a FCN preprocessor sub-network to a public TCIA head and neck cancer dataset. The training goal is survival prediction of radiotherapy cases based on pre-treatment FDG PET-CT scans, acquired across 4 different hospitals. We show that the preprocessor sub-network in conjunction with aggregated residual connection leads to improvements over state-of-the-art results when combining both CT and PET input images.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge