Roberto A Novoa
Disparities in Dermatology AI Performance on a Diverse, Curated Clinical Image Set
Mar 15, 2022Abstract:Access to dermatological care is a major issue, with an estimated 3 billion people lacking access to care globally. Artificial intelligence (AI) may aid in triaging skin diseases. However, most AI models have not been rigorously assessed on images of diverse skin tones or uncommon diseases. To ascertain potential biases in algorithm performance in this context, we curated the Diverse Dermatology Images (DDI) dataset-the first publicly available, expertly curated, and pathologically confirmed image dataset with diverse skin tones. Using this dataset of 656 images, we show that state-of-the-art dermatology AI models perform substantially worse on DDI, with receiver operator curve area under the curve (ROC-AUC) dropping by 27-36 percent compared to the models' original test results. All the models performed worse on dark skin tones and uncommon diseases, which are represented in the DDI dataset. Additionally, we find that dermatologists, who typically provide visual labels for AI training and test datasets, also perform worse on images of dark skin tones and uncommon diseases compared to ground truth biopsy annotations. Finally, fine-tuning AI models on the well-characterized and diverse DDI images closed the performance gap between light and dark skin tones. Moreover, algorithms fine-tuned on diverse skin tones outperformed dermatologists on identifying malignancy on images of dark skin tones. Our findings identify important weaknesses and biases in dermatology AI that need to be addressed to ensure reliable application to diverse patients and diseases.
Disparities in Dermatology AI: Assessments Using Diverse Clinical Images
Nov 15, 2021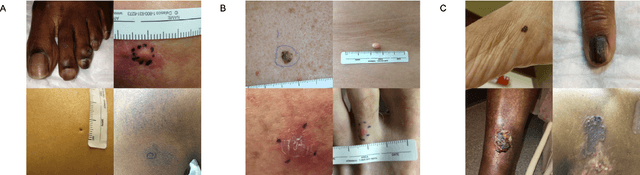
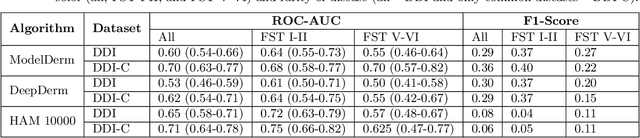

Abstract:More than 3 billion people lack access to care for skin disease. AI diagnostic tools may aid in early skin cancer detection; however most models have not been assessed on images of diverse skin tones or uncommon diseases. To address this, we curated the Diverse Dermatology Images (DDI) dataset - the first publicly available, pathologically confirmed images featuring diverse skin tones. We show that state-of-the-art dermatology AI models perform substantially worse on DDI, with ROC-AUC dropping 29-40 percent compared to the models' original results. We find that dark skin tones and uncommon diseases, which are well represented in the DDI dataset, lead to performance drop-offs. Additionally, we show that state-of-the-art robust training methods cannot correct for these biases without diverse training data. Our findings identify important weaknesses and biases in dermatology AI that need to be addressed to ensure reliable application to diverse patients and across all disease.
TrueImage: A Machine Learning Algorithm to Improve the Quality of Telehealth Photos
Oct 01, 2020

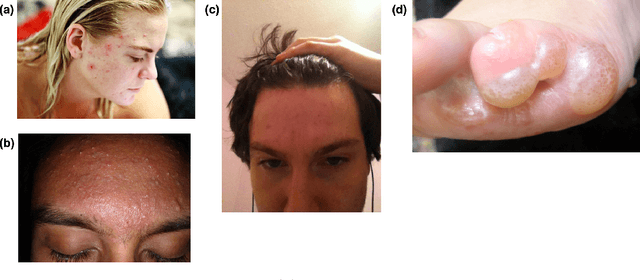

Abstract:Telehealth is an increasingly critical component of the health care ecosystem, especially due to the COVID-19 pandemic. Rapid adoption of telehealth has exposed limitations in the existing infrastructure. In this paper, we study and highlight photo quality as a major challenge in the telehealth workflow. We focus on teledermatology, where photo quality is particularly important; the framework proposed here can be generalized to other health domains. For telemedicine, dermatologists request that patients submit images of their lesions for assessment. However, these images are often of insufficient quality to make a clinical diagnosis since patients do not have experience taking clinical photos. A clinician has to manually triage poor quality images and request new images to be submitted, leading to wasted time for both the clinician and the patient. We propose an automated image assessment machine learning pipeline, TrueImage, to detect poor quality dermatology photos and to guide patients in taking better photos. Our experiments indicate that TrueImage can reject 50% of the sub-par quality images, while retaining 80% of good quality images patients send in, despite heterogeneity and limitations in the training data. These promising results suggest that our solution is feasible and can improve the quality of teledermatology care.
 Add to Chrome
Add to Chrome Add to Firefox
Add to Firefox Add to Edge
Add to Edge